If you’ve ever booked an online skin appointment and wondered whether it’s “telehealth” or “telemedicine,” you’re not alone. People use the words like they mean the same thing. But the difference matters when you’re trying to get the right kind of help, especially for dermatology (skin, hair, and nail care). This guide breaks down telehealth vs telemedicine in plain English. You’ll learn what each term means, what kinds of services fall under each one, and how common online dermatology options like teledermatology fit in. And because labels don’t treat rashes, we’ll also talk through what you can and can’t realistically handle online.
Best for: People who want a clear, practical way to tell online medical visits from broader remote health support.
Not ideal when: You have severe pain, fast-spreading swelling, heavy bleeding, or symptoms that feel like an emergency.
Good first step if: You’re not sure whether you need a diagnosis and prescription or just guidance, education, or follow-up support.
Call a pro if: Your skin issue is changing quickly, looks infected, involves eyes/genitals, or you’re worried it could be cancer.
Quick Summary
-
Telemedicine is remote clinical care, like a diagnosis, treatment plan, or prescription through video, phone, or messages.
-
Telehealth is the bigger umbrella. It can include telemedicine plus education, scheduling, monitoring, and care coordination.
-
Teledermatology is dermatology delivered remotely. It can be telemedicine (diagnosis) or telehealth (follow-up support).
-
Online care works best when photos are clear and your symptoms can be described well.
-
Some problems still need hands-on exams, in-office procedures, labs, or urgent in-person care.
Telehealth vs Telemedicine at a Glance
Telemedicine is a subset of telehealth. An easy memory aid is: telemedicine treats, telehealth supports. Telemedicine focuses on direct clinical services like diagnosis and treatment, including prescription starts, stops, and refills. Telehealth includes that, plus education, care coordination, and remote patient monitoring.
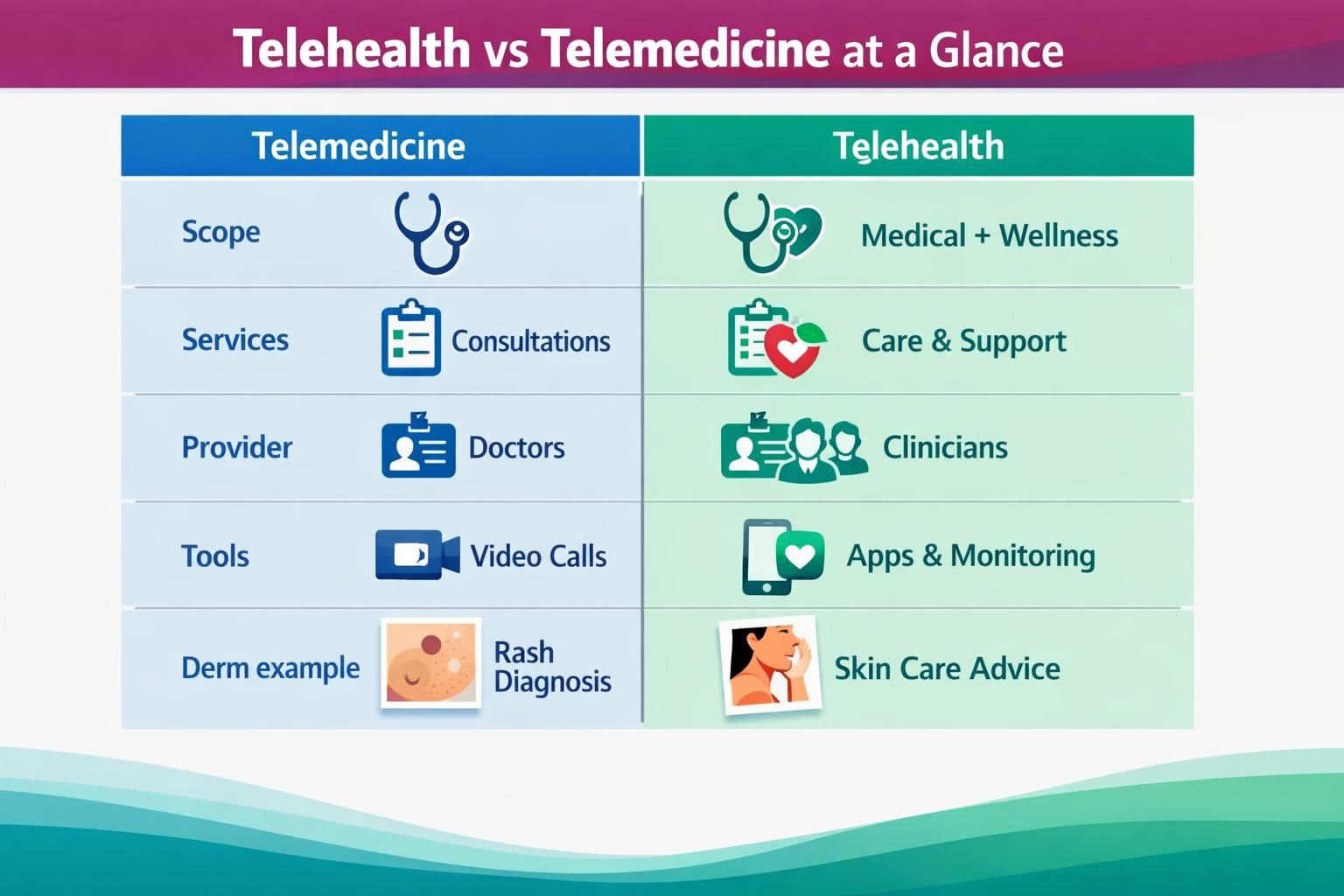
For an online derm visit, sending rash photos for a diagnosis and medication plan is usually telemedicine. Help with routines, trigger tracking, or follow-up logistics is usually telehealth.
Related term: telecare, which is often non-clinical check-ins or safety monitoring rather than diagnosis.
One-sentence Definitions
Telemedicine: remote clinical services where a licensed clinician evaluates you and provides care, like diagnosis, treatment, and prescriptions.
Telehealth: the broader category of health-related services delivered at a distance, including telemedicine plus education, monitoring, admin support, and public health services.
Teledermatology: dermatology delivered remotely, either as telemedicine (clinical consultation and treatment) or telehealth (support and follow-up).
Telecare: remote support services that help you manage health and safety, often without direct medical diagnosis or prescribing.
Quick Comparison Table
TypeWhat it coversCommon toolsDermatology exampleTelemedicineDiagnosis and treatmentVideo, phone, photo reviewAcne visit with prescriptionTelehealthWider health servicesPortals, apps, messagingCare plan reminders and educationTelecareSupport and check-insCalls, alerts, monitoringNon-clinical follow-up check-in
What is Telemedicine?
Telemedicine is medical care delivered remotely by a clinician who can assess symptoms and make clinical decisions. It’s a real medical visit, just not in the same room. The clinician takes a history, asks questions, and documents the encounter in an electronic health record (EHR).
Telemedicine can be video, phone, or secure asynchronous messaging. In dermatology, “store-and-forward” is common: you send photos and details first, then the clinician reviews them later.
It works best when the problem can be seen or described clearly. Limits remain: cameras can’t feel a lump, confirm vitals, or do procedures like biopsies.
Common Telemedicine Examples
Telemedicine commonly includes clinical tasks that end with a medical decision. Examples include:
-
A clinician reviews photos of a new rash and gives a diagnosis plus a treatment plan.
-
A follow-up appointment to adjust acne medication or eczema cream strength.
-
Prescription management for refills or side effect checks.
-
Triage, meaning deciding whether you can stay home, need an urgent visit, or should go to the emergency room.
-
A skin check concern where you’re told to come in promptly because a spot looks suspicious. If you’re comparing a new spot, telling harmless marks apart can help you describe what you’re seeing.
What is Telehealth?
Telehealth is the umbrella term for delivering health-related services at a distance. It includes telemedicine plus the support systems around care. That can include patient education, care coordination, public health services, and even provider training.
Telehealth often uses a platform for video, secure messaging, and file sharing, plus a patient portal where you view results and manage appointments. Mobile health apps can also count when they connect to your care team.
In dermatology, telehealth may include coaching on topical use, reminders for follow-up photos, and guidance on triggers and routines.
Common Telehealth Examples (Including Non-clinical)
Telehealth goes beyond clinical diagnosis. Common examples include:
-
Appointment scheduling and reminders through a patient portal.
-
Care coordination, like sharing notes between your primary care clinician and a dermatologist.
-
Patient education, such as how to use steroid creams safely or how to protect your skin barrier. If you’re sorting product types, choosing the right eczema cream is a useful companion read.
-
Behavioral health services delivered online, like counseling for stress that worsens skin picking or psoriasis flares.
-
Provider training, such as clinicians learning a new telehealth platform workflow.
-
Public health services, like remote outreach and education during community health campaigns.
Key Differences (Scope, Services, and Technology)
Telemedicine is remote clinical care: diagnosis, treatment, and medical decision-making. Telehealth is broader and includes telemedicine plus services that support ongoing care, like education, messaging, and chronic-care coordination. The tech can look similar, but the aim differs: telemedicine tools prioritize safe decisions, while telehealth tools prioritize continuity.
In dermatology, a clinician reviewing a mole photo and advising next steps is telemedicine. Help building a skin-care routine or coordinating follow-ups is telehealth. For a fast-changing lesion, you may need in-person care. See fast-appearing skin cancer concerns.
Synchronous vs Asynchronous Care
Synchronous care means real-time interactive care, like a live video visit or a phone visit where you talk back and forth. It’s best when your clinician needs to ask follow-up questions on the spot, like “Does it itch or burn?” or “Does it blanch when you press it?”
Asynchronous care means you send information first and the clinician responds later. In dermatology, that often means store-and-forward: you upload photos and a symptom history, then get a clinical consultation after review. This works well for acne, eczema, and many straightforward rashes because high-quality images can be more useful than shaky video.
A practical tip: good lighting and sharp photos matter. Think of it like trying to buy something online. If the picture is blurry, everyone’s guessing.
Remote Patient Monitoring (RPM) and Where it Fits
Remote patient monitoring (RPM) is the ongoing collection of health data outside the clinic and sharing it with a care team over time. It usually falls under telehealth, not telemedicine, because it’s monitoring rather than a single decision-making visit.
RPM may use home devices or wearables such as blood pressure cuffs, pulse oximeters, glucose monitors, or, in some programs, digital stethoscopes. Data often flows through an app into the EHR.
Dermatology uses RPM less, but similar tracking shows up when you log flare triggers, submit serial photos, or track adherence for weeks.
Legal, Privacy, and Reimbursement Considerations (U.S.)
In the U.S., telehealth rules affect what clinics can provide online, how your data must be protected, and whether insurers reimburse the visit. Requirements vary by state, payer, and clinic, so policies differ and booking options can be limited.
Privacy matters: visits and messaging should use secure, compliant systems, not standard social media or personal texting. Many clinics also require informed consent, meaning you agree to remote care after hearing the limits and alternatives.
Reimbursement shapes access. Services that payers cover consistently are offered more widely, while others may be restricted or reserved for established patients.
HIPAA and Data Security Basics
HIPAA (Health Insurance Portability and Accountability Act) is the main U.S. privacy law that sets rules for protecting your medical information. In plain terms, it’s about keeping your health data private and controlled.
Data security is the practical side. It includes encryption (scrambling data so outsiders can’t read it), secure logins, and controlled access inside the clinic. A telehealth platform and patient portal are usually built with these protections in mind.
You can do your part too:
-
Use a private Wi-Fi network when possible.
-
Don’t share screenshots of your visit.
-
Ask where photos are stored and who can see them.
-
Keep your app and phone updated, since updates often fix security issues.
Licensing Across State Lines (High-level)
Clinicians generally need a license in the state where the patient is located during the visit. That makes cross-state tele-visits complicated. If your dermatologist is licensed in one state and you’re physically in another, the clinic may be limited, especially for prescribing.
Some organizations use multi-state licenses, compacts, or telehealth allowances, but the practical rule is: your location at the time of care matters more than your home address.
When traveling, you may get general guidance but not medication. Plan ahead for refills. For flare discussions, what Benadryl really does can help.
When to Choose Telemedicine vs Telehealth
Choose telemedicine when you need a clinician to evaluate a specific problem and make a medical decision. Choose telehealth when you need broader support around care, like education, monitoring, or coordination. In dermatology, telemedicine fits “What is this?” and “What should I use?” Telehealth fits “How do I stick with this plan?” and “What are my next steps?”
Use this quick filter: diagnosis, prescription, or documentation usually means telemedicine. Education, coaching, and follow-up logistics usually means telehealth.
Skip both if you have rapidly spreading redness, fever, pus, facial swelling near the eyes, trouble breathing, or a fast-changing mole. Provide clear photos, a timeline, and your medication list.
Best Use Cases for Patients
The best use case is the one that matches your goal and your risk level. Practical examples:
-
Telemedicine: acne evaluation, eczema flare assessment, medication adjustments, straightforward dermatitis, and telemedicine vs telehealth dermatology questions where you need an actual treatment decision.
-
Telehealth: routine education on triggers, skin-care routine troubleshooting, appointment scheduling, and care coordination after an in-person procedure.
-
Either one can support teledermatology, depending on whether it’s clinical decision-making or ongoing support.
A quick checklist before you book:
-
Can you take clear photos in good light?
-
Do you know when it started and what you’ve tried?
-
Are you on medications that matter for skin (like steroids or immunosuppressants)?
-
Is there any chance this is urgent or needs a procedure?
Conclusion
Telehealth vs telemedicine isn’t a trivia question. It changes what kind of help you’re actually signing up for, especially with teledermatology. Telemedicine is the clinical visit part, like diagnosis, treatment plans, and prescription management. Telehealth is the bigger umbrella that can include education, coordination, portals, and monitoring. Your next step is simple: decide whether you need a medical decision or support around care, then book the option that matches. If anything feels urgent, fast-changing, or hard to capture on camera, skip the online route and get seen in person.