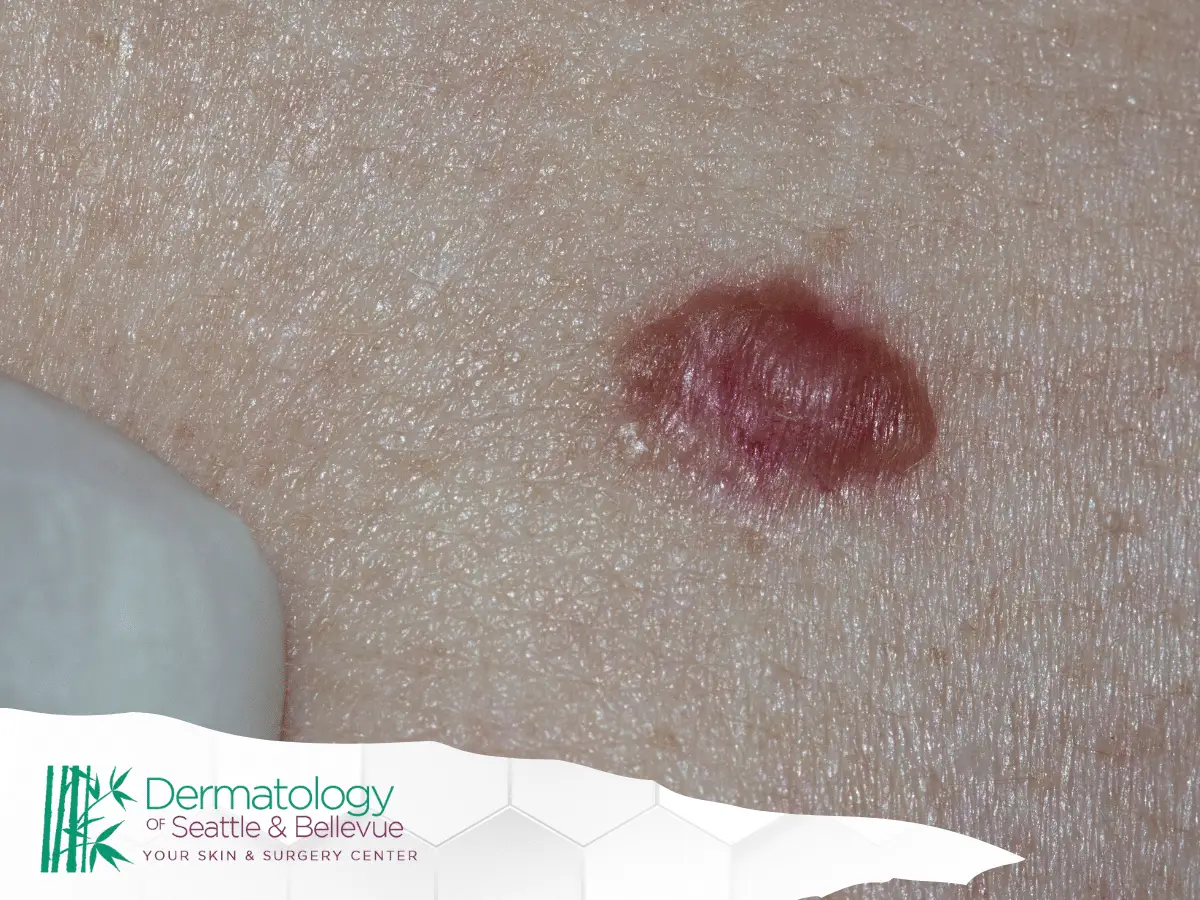
Can Basal Cell Carcinoma Come Back In The Same Spot?
Quick Summary
- Basal cell carcinoma (BCC) can return in the same spot, especially if microscopic cells remain after treatment.
- Recurrence risk rises with infiltrative or morpheaform subtypes, genetics, and ongoing UV exposure.
- Watch the treated area for new lesions, persistent scarring, or skin texture/color changes; biopsies confirm recurrence.
- Treatment options include excision, Mohs surgery, ED&C, cryotherapy, radiation, topical meds, and hedgehog inhibitors for advanced cases.
- Sun protection and regular dermatology follow-ups help reduce recurrence risk and catch problems early.
Many individuals diagnosed with this common form of skin cancer are concerned about the recurrence of basal cell carcinoma (BCC) in the same spot. While treatment may successfully eliminate visible signs of the tumor, the potential for BCC to return to the same location raises questions about long-term management and surveillance.
Here, we delve into the factors influencing BCC recurrence, strategies for monitoring, and the importance of proactive care.
Understanding Recurrence Risk:
Despite effective treatment, BCC can recur in the same spot due to various factors, including incomplete tumor removal, genetic predisposition, and ongoing sun exposure.
In some cases, microscopic cancer cells may remain in the surrounding tissue following initial treatment, increasing the risk of recurrence over time.
Additionally, certain subtypes of BCC, such as infiltrative or morpheaform variants, are associated with a higher likelihood of local recurrence.
Monitoring for Recurrence:
Regular skin examinations are crucial for detecting early signs of BCC recurrence in the same spot. Patients should remain vigilant for changes in the treated area, including the appearance of new lesions, persistent scarring, or alterations in skin texture and color. Dermatologists can perform thorough examinations and, if necessary, biopsy suspicious lesions to confirm recurrence.
Treatment for Basal Cell Carcinoma (BCC)
Treatment for Basal Cell Carcinomas (BCC) involves a multifaceted approach to effectively eliminate skin cancer cells while preserving optimal cosmetic and functional outcomes.
Treatment choice depends on various factors, including the tumor size, location, subtype, depth of invasion, and the patient’s overall health and preferences.
Here, we explore the diverse treatment modalities available for BCC and their respective indications:
Surgical Excision:
Surgical excision is the primary treatment for most cases of BCC, particularly those with well-defined borders and minimal invasion.
During the procedure, the tumor is surgically removed along with a margin of surrounding healthy tissue to ensure complete eradication.
Techniques such as Mohs micrographic surgery offer high cure rates while minimizing tissue loss and preserving cosmetic appearance, making them ideal for tumors in aesthetically sensitive areas or those with high recurrence risk.
Mohs Micrographic Surgery:
Mohs micrographic surgery is a specialized technique that involves precise removal of BCC layers, followed by immediate microscopic examination of the excised tissue margins.
This iterative process continues until no skin cancer cells are detected, ensuring maximal tumor removal while sparing healthy tissue. Mohs surgery is particularly suited for large, recurrent, or high-risk BCCs and lesions located in cosmetically sensitive or functionally critical areas.
Curettage and Electrodesiccation (ED&C):
Curettage and electrodesiccation (ED&C) is a less invasive treatment option suitable for small, superficial BCC lesions.
The procedure involves scraping the tumor with a curette to remove the visible portion, followed by cauterization of the tumor bed with an electric current to destroy the remaining skin cancer cells. ED&C is generally reserved for low-risk BCCs on the trunk or extremities and may require multiple sessions for complete clearance.
Cryotherapy:
Cryotherapy involves freezing BCC lesions with liquid nitrogen to induce cell death and tumor destruction.
This technique is typically employed for small, superficial BCCs or in patients who are poor candidates for surgery due to medical comorbidities or cosmetic concerns.
Cryotherapy is convenient, cost-effective, and associated with minimal scarring but may require repeated treatments for optimal efficacy.
Radiation Therapy:
Radiation therapy, including external beam radiation therapy (EBRT) and brachytherapy, may be recommended for patients with unresectable or high-risk BCC lesions.
Radiation delivers targeted energy to the tumor site, destroying cancer cells while minimizing damage to surrounding healthy tissue. Radiation therapy is particularly useful for elderly patients, those with multiple comorbidities, or lesions located in anatomically challenging areas.
Topical Therapies:
Topical medications such as imiquimod or 5-fluorouracil (5-FU) may be prescribed for superficial BCC lesions or patients who prefer non-invasive treatment options.
These medications stimulate the body’s immune response to target and eliminate cancer cells, leading to localized skin reactions and eventual tumor clearance.
Topical therapies are most suitable for low-risk BCCs on the trunk, extremities, or face and may require several weeks to months of treatment.
Targeted Therapy:
Hedgehog pathway inhibitors, such as vismodegib and sonidegib, are oral medications approved for treating locally advanced or metastatic BCC. These targeted therapies block aberrant signaling pathways involved in BCC development and progression, effectively inhibiting tumor growth and inducing regression.
Targeted therapy is indicated for patients with advanced or unresectable BCCs who are not candidates for surgery or radiation therapy.
By tailoring treatment approaches to individual patient characteristics and tumor characteristics, healthcare providers can effectively manage BCC while optimizing outcomes and minimizing the risk of recurrence and metastasis.
Preventive Measures:
Individuals should adopt sun protection measures and minimize exposure to harmful ultraviolet (UV) radiation to reduce the risk of BCC recurrence in the same spot.
This includes wearing protective clothing, applying broad-spectrum sunscreen, seeking shade during peak sunlight hours, and avoiding indoor tanning devices.
By practicing sun-safe behaviors, patients can help prevent new BCC lesions from developing and reduce the likelihood of recurrence.
The Role of Ongoing Surveillance:
Following treatment for BCC, regular follow-up appointments with a dermatologist are essential for ongoing surveillance and early detection of recurrence.
These appointments may include comprehensive skin examinations, discussion of any concerning symptoms or changes, and education on skin cancer prevention and self-monitoring techniques.
Regular follow-up and surveillance are essential for monitoring treatment response, detecting recurrence, and ensuring long-term skin health and well-being.
Final Words
In conclusion, while this blog provides valuable information on the treatment options for Basal Cell Carcinoma (BCC), it’s essential to remember that each case is unique. It is crucial for patients to consult with a healthcare professional to determine the best course of action tailored to their specific condition. Ignoring symptoms can lead to serious ramifications, including the potential consequences of untreated basal cell carcinoma, which may involve deeper tissue damage and increased risk of more aggressive cancers. Regular check-ups and early intervention can make a significant difference in outcomes and overall health. Additionally, patients should be aware of the basal cell carcinoma metastasis risk, as this can vary depending on individual factors such as the size and location of the tumor. Early recognition and treatment not only help prevent complications but also reduce the likelihood of more severe health issues in the future. By staying informed and proactive, patients can significantly improve their chances of a successful recovery and maintain their quality of life.
Consulting with a qualified healthcare provider is crucial for the most accurate assessment and personalized treatment plan tailored to your specific needs.
Don’t hesitate to schedule an appointment with a dermatologist or oncologist to discuss your concerns, explore all available options, and receive expert guidance on managing BCC effectively.
Your health and well-being are paramount; seeking professional medical advice is the best way to ensure optimal outcomes.