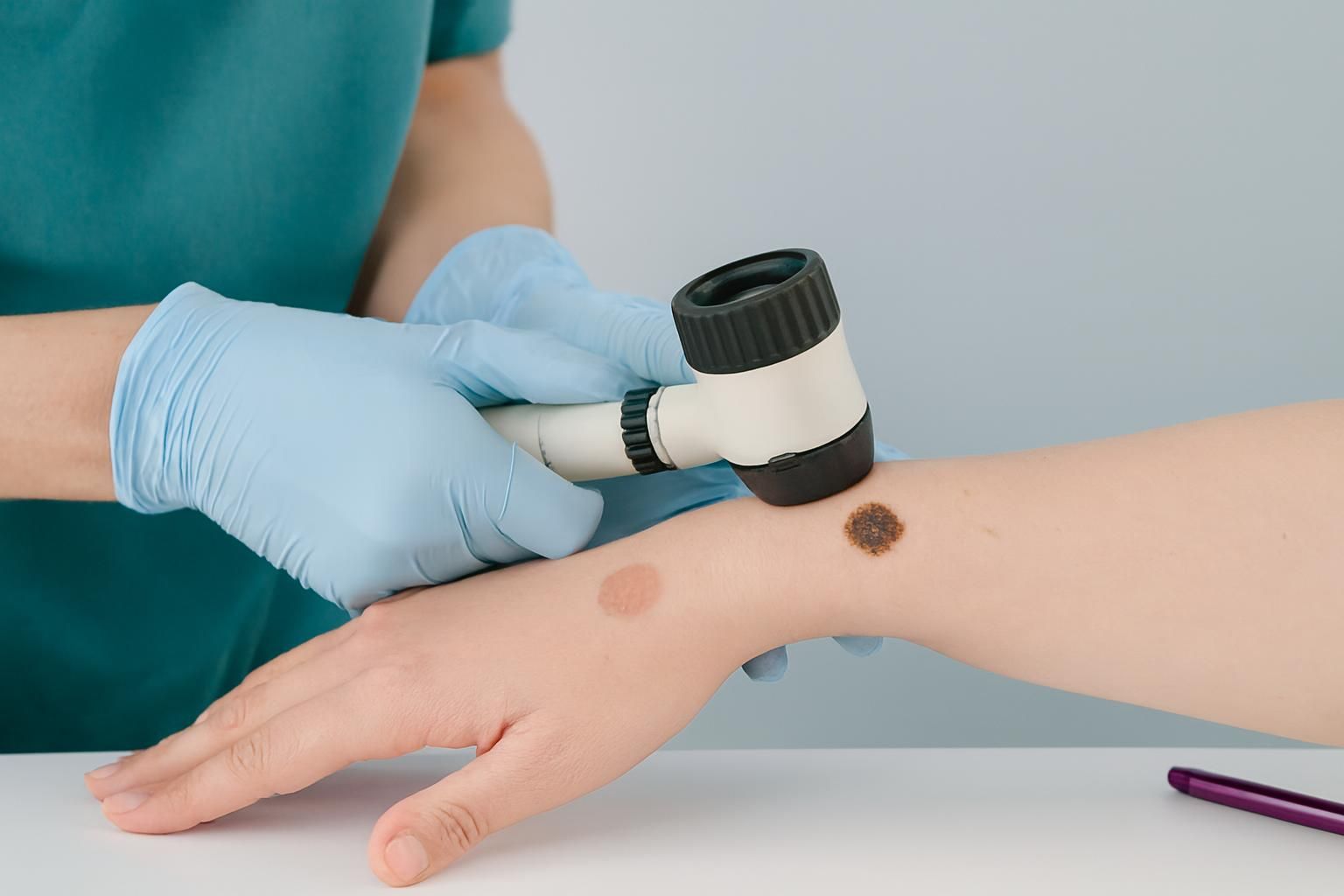
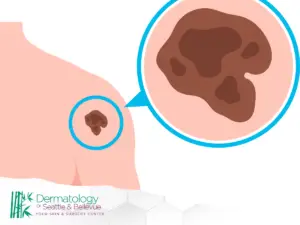
Noticing a new spot on your skin or a change in one you have had for years can be unsettling, especially when you start wondering about melanoma vs birthmark. Many marks are harmless, but some changes deserve prompt attention because early detection matters. This guide explains what birthmarks and moles typically are, what melanoma is, and the visual clues that can help you decide whether a spot should be checked. You will also learn how location, color, shape, and change over time can point toward a benign birthmark or something more concerning, plus what to do next and what to expect at a skin exam.
- Birthmarks are usually stable, long-standing skin changes, while melanoma is a type of skin cancer that tends to evolve.
- The most useful red flag is change: growth, new colors, new symptoms, or a new spot that looks unlike your others.
- Use the ABCDE approach and the “ugly duckling” idea to spot lesions that warrant evaluation.
- Some marks can resemble each other, so uncertainty is a reason to get a professional skin check.
- Photos and simple tracking can make it easier to notice meaningful changes over time.
What counts as a birthmark, a mole, or melanoma?
A birthmark is a skin mark present at birth or appearing shortly after. Birthmarks can be pigmented (tan, brown, blue, gray) or vascular (pink, red, purple), and may be flat or raised. Many stay consistent, though some fade or change texture with age. A mole is a common pigmented spot caused by clusters of pigment-producing cells; moles may be present early or develop over time.
Melanoma is a cancer that arises from pigment-producing cells. It can develop in an existing mole or appear as a new lesion on normal skin. It often draws attention because it changes, looks irregular, or behaves differently than a typical mole. In the melanoma vs birthmark question, timing and behavior matter: birthmarks and many benign moles are usually steady, while melanoma more often evolves.
Why “change over time” matters most
Stability is reassuring. Some gradual, symmetric growth can happen as the body grows, especially in childhood and adolescence, but adult-onset change deserves more attention. Melanoma tends to be dynamic, with shifts in size, shape, border, or color over weeks to months, though changes can be subtle.
A mark that has looked the same for years and becomes slightly drier or mildly raised with normal aging is often less concerning than a spot that develops new irregularity, multiple colors, bleeding without a clear cause, or a persistent sore. If you are unsure, document the spot and book an exam rather than waiting.
Visual clues: ABCDE and the “ugly duckling” sign
The ABCDE approach is a practical way to screen pigmented lesions at home. It does not diagnose anything, but it can help you flag spots that should be evaluated. Use good lighting, a mirror, and photos for comparison. Focus on what is new, changing, or distinctly different from the rest of your spots.
The “ugly duckling” sign is a helpful shortcut: most people’s moles share a family resemblance. One spot that looks unlike your others, even if it does not fit every ABCDE point, can be worth a closer look, especially if you have many moles.
ABCDE: what each letter means in real life
A is for Asymmetry: one half does not match the other. Many benign moles are fairly symmetric. Asymmetry may show up as a lopsided outline or uneven color placement.
B is for Border: edges that are irregular, scalloped, blurry, or notched. Benign lesions often have smoother borders, though not always. A border that seems to spread into surrounding skin is a caution sign.
C is for Color: more than one color or uneven color. Watch for mixtures of brown, black, gray, blue, red, or white within one lesion. Uniform tan or brown is more typical of benign moles; multiple shades can be a warning sign.
D is for Diameter: larger spots can be more concerning, but size alone is not decisive. Small lesions can still be melanoma, and some benign lesions can be large.
E is for Evolving: change in size, shape, color, elevation, or symptoms such as itching, tenderness, crusting, or bleeding.
The “ugly duckling” approach for people with many spots
If you have numerous moles, most may look similar (for example, small, round, light-brown dots). The ugly duckling is the one that breaks your pattern: darker, more irregular, more raised, or simply different. This can be useful when a long-standing patch starts to look unlike your baseline.
Do a quick scan of an area and ask whether any one spot immediately draws your eye. If yes, take a photo and compare it with older photos if available. Consider asking someone else to look, since fresh eyes can catch differences. If you cannot confidently categorize the spot, get a professional opinion.
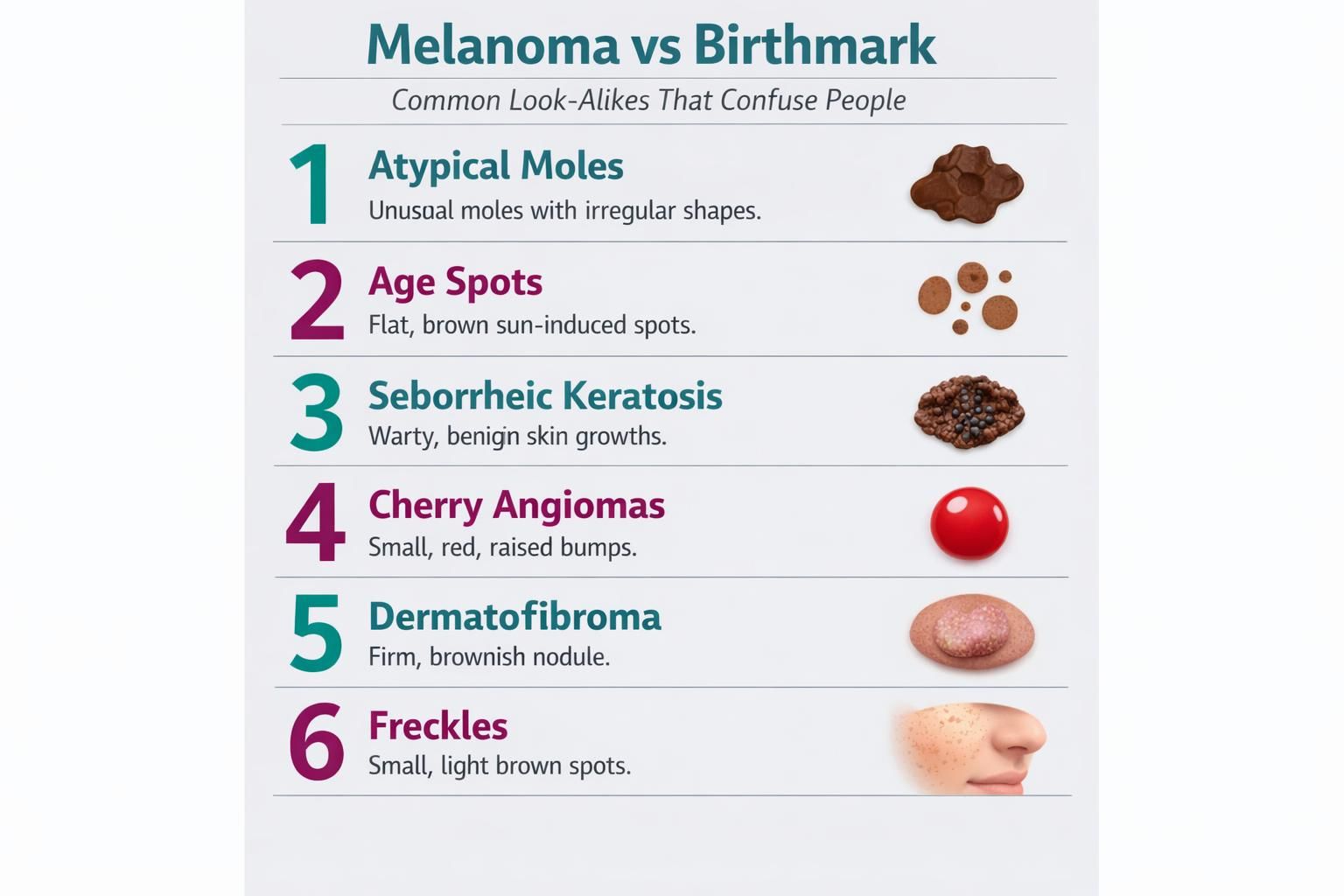
Common look-alikes that confuse people
Many benign marks can mimic concerning features, and not every irregular border or color variation is dangerous. Some harmless lesions appear later in life. At the same time, melanoma does not always look like a classic dark mole and may include red, pink, or lighter areas.
Because overlap is common, this section is not meant to diagnose. If a lesion is changing, symptomatic, or hard to categorize, that uncertainty alone is a reasonable reason to book an exam.
Pigmented birthmarks vs. atypical moles
Pigmented birthmarks are often flat patches with fairly even color, though they can vary and may be larger than common moles. Some have hair growth. Atypical moles (dysplastic moles) can have irregular borders and varied color and still be benign, which is why one feature is rarely enough to decide.
Clues that lean benign include long-term stability, relative symmetry, and a consistent pattern compared to your other moles. Clues that lean concerning include new irregularity, a new darker focus within a larger patch, or rapid change. If a pigmented patch you have always considered a birthmark develops a new raised area or a new color, it should be examined.
Vascular birthmarks and red flags
Vascular birthmarks are usually pink, red, or purple and come from blood vessel changes. They may blanch when pressed, appear as a flat stain, or feel more textured. These lesions often have a long, consistent history. Bleeding can happen from friction or minor injury, not only from cancer.
Red flags include a new lesion that grows quickly, ulcerates, repeatedly bleeds without clear trauma, or forms a persistent crust or sore. Another warning sign is a spot that never fully heals. Even if the cause is benign, ongoing symptoms warrant assessment.
Shape questions: what about heart shaped moles?
Heart shaped moles can be benign, and shape alone is not a diagnosis. Some spots look heart-like because of a small notch or indentation, and their distinct look can make them easier to monitor. If a mole has always been heart shaped and remains stable in size, border, and color, that consistency is generally reassuring.
Concern rises if the “heart” appearance reflects increasing border irregularity or if one side changes more than the other. Watch for evolution: a deepening notch, edges becoming jagged, or new colors appearing. If you are tracking a distinctive mole, take periodic photos using similar distance and lighting so changes are easier to detect and describe.
Can birthmarks be cancerous? Understanding risk without panic
The question can birthmarks be cancerous has a nuanced answer. Most birthmarks are benign and never become cancer. However, any skin lesion can be involved in cancer in a few ways: cancer can arise within a lesion, a lesion can be mistaken for cancer, or cancer can appear nearby and be overlooked because attention stays on the “birthmark.” That is why change and new symptoms matter more than the label.
If you have a large pigmented birthmark, or one that is hard to monitor because of its location, routine professional skin checks can help. The goal is not to assume risk but to make monitoring more reliable. Regardless of your baseline, a new lesion that looks different from your other marks, or a longstanding lesion that evolves, deserves evaluation.
What to do if you are worried: self-checks, photos, and when to book an exam
Start with a simple system rather than frequent checking. Do a monthly or periodic head-to-toe scan, including the scalp, behind the ears, under the breasts, between fingers and toes, and the soles of the feet. Use mirrors or ask a partner to help. If you find a spot of concern, take clear photos and note the date, location, and symptoms. Include a ruler or coin for scale if helpful.
Consider booking an exam if you notice any of the following:
- A spot that is new and looks unlike your other moles
- A lesion that is changing in size, shape, border, or color
- Bleeding, crusting, or a sore that does not heal
- Persistent itching, tenderness, or pain in a specific spot
- A new dark area within an older patch, or a new raised bump in a flat lesion
During an appointment, a clinician may examine the spot closely and decide whether it can be monitored or should be sampled. If a biopsy is recommended, it is typically done to get clarity, not to assume the worst. Bring your photos and your timeline, since your history of change can be as informative as the spot itself.
Conclusion
Sorting out melanoma vs birthmark comes down to patterns, change, and professional confirmation when the picture is unclear. Birthmarks and many moles are stable features of your skin, while melanoma is more likely to evolve, develop irregular borders, show multiple colors, or stand out as an “ugly duckling.” If you are concerned about a melanoma birthmark possibility, avoid guessing based on a single feature and focus on whether the lesion is changing or symptomatic. Your next step is practical: take a clear photo, note what you are seeing, and schedule a skin exam if any red flags are present. Early evaluation is the fastest path to reassurance or timely care.